I came across a really encouraging article about tech start-ups that are trying to fix the elderly caregiving sector. This is incredibly important work.
The double whammy is here
The graphic below, from the UN, shows how our global population is aging. It will happen faster in developed countries. In Japan people above 65 already constitute more than a quarter of the population. Singapore will get there in the 2030s, and the U.S. in the 2040s.
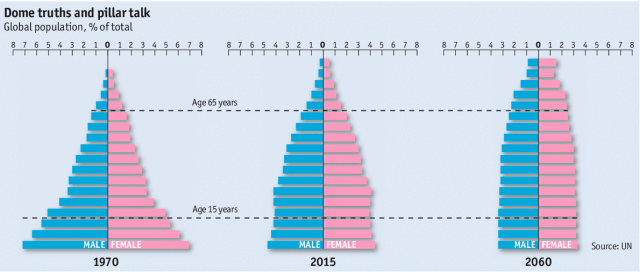
This will be a double whammy on societies. Countries will have a shrinking tax base to support the growing number of elderly who need care. There won’t be abundant resources to build new nursing homes and hospital beds. At the same time, it will be more difficult for the elderly to continue living at home – with shrinking family sizes, the responsibility for caregiving will fall on one or two children, instead of three or four.
Advances in biotechnology, personalised medicine and genomics will go a long way towards mitigating these challenges. For example, if companies like Calico and Unity Biotechnology manage to reverse aging, people can have longer, healthier, independent lives. The periods of time when they need caregiving will plummet. This is referred to as a longer “healthspan” (as opposed to just “lifespan”).
Unfortunately, many developed countries are already starting to face the double whammy and need a more immediate solution. From a policy perspective, it does not make sense to build new infrastructure for the elderly because these will become redundant when subsequent elderly cohorts are smaller.
The best solution is to help people receive care in their own homes as they age. It is also what a large majority (some statistics suggest 90%) of people prefer.
Why is Home Caregiving such a tough nut to crack?
A fragmented home care sector with low standards and revolving door caregivers is the norm in many cities. I don’t see a level of innovation and investment flowing into this sector that is commensurate to its importance. Three likely reasons why this is such a tough nut to crack.
- Home caregiving is highly personal. When someone takes an Uber ride, they don’t have to talk to the driver if they don’t want to. In contrast, a caregiver gets deep into your personal space if they bathe, feed and change your diaper. You’re obviously going to be very picky about who you choose. Pickiness is not a one-way street – caregivers have their preferences too!
- The Home caregiving sector suffers from “diseconomies of scale”. A service like Uber gets more efficient as more drivers and users come on board. It works the other way with caregiving because scale creates a more complex landscape of preferences, and a higher probability of error. According to Seth Sternberg, CEO of Honor (a caregiving start-up) “an agency with fewer than 100 carers can match them with clients and schedule their appointments with relative ease, but if it tries to get bigger, things go wrong. The agency ends up making poor matches… an obese client who owns kittens might end up being sent a petite woman who is allergic to cats… and when schedulers start arranging appointments outside of a small geographic area they know well, caregivers end up being late or not turning up at all.”
- The job is just not a lot of fun. In fact, that’s why many people out-source care to paid contractors, even care for those they love most. It’s not glamorous, it’s repetitive, it can be highly physical, and in some cases, you interact with suffering on a daily basis. For such a difficult job, you mostly work alone without a network of support and accountability. Benefits, training and wages are patchy. Motivation is low. It is more difficult to recruit a good part-time Caregiver than a good part-time Uber driver.
What are the implications for tech companies and smart cities?
Disrupting the flailing home care sector is a classic problem that the tech, business, Government and non-profit sectors need to go at together. Here are three things that anyone working in this space needs to consider.
- Tackle the root problem – motivation.
The FT article features Josh Bruno,who left Bain Capital to set up Hometeam. He started with a tech solution in mind – perhaps the equivalent of Uber for in-home care, he thought – a platform that would match caregivers to elderly and take a cut.
After volunteering in about 40 elderly care organisations, he quickly realised that the deepest issue in the caregiving sector was not matching, but motivation – “People blame them as lazy, but they are the worst working conditions — low pay, no training.” Defying all industry standards, he decided to hire the caregivers, give them good benefits of paid holidays, maternity leave, training and retirement.
I think Josh is getting to the heart of the issue – how can you expect people to deliver quality care if you don’t care for them? The first step is turn caregiving into a worthy career. Business can’t tackle this alone, which leads me to point two.
2. Partner to make home care an economically viable business
Josh’s company was turned away by many VCs because hiring the caregivers was not deemed to be maximally profitable.
I believe many have not yet realized the economic benefits of a strong home care sector. When elderly are able to continue living in their own homes, a whole ecosystem of services such as tele-health, food delivery and transport has a larger market. For large healthcare providers like Kaiser Permanente, a strong home care sector combined with tele-health can help manage its elderly clients outside the expensive hospital setting. This optimizes the use of hospital facilities and doctors’ time, making the business more profitable. For the same reasons, countries where healthcare systems are operated by the Government should consider investing public funds in the home care space, for example, by extending subsidies in nursing homes to the home care sector.
Furthermore, to help the home care sector grow, the public and non-profit sectors should play a role in helping to overcome inherent”diseconomies of scale”. It does not make sense for small home care companies to have their own training programmes and qualifications system. One idea is for Governments or non-profits to offer basic, modularised caregiver training as a “shared resource” for home care companies to utilise.
3. Use technology to build a care ecosystem around the elderly
Although it may not currently feel like it, home caregivers are really part of a team of family members, healthcare professionals and community members who help make living at home comfortable and enjoyable.
Technology can enable better communication and support between different members of this team. The home caregiver should be able to ask the healthcare professional whether a situation requires medical attention, and share information that would help the healthcare professional with diagnosis and prescription. Community members should be able to volunteer in bite-sized chunks of time, a topic I wrote about in my article “Three ways to build a transportation system that services the vulnerable”. Ultimately, when members of the team communicate, they can collectively give better care and receive support from each other. This can help to tackle the motivation problem for caregivers.
Technology can be part of the care team too! It can enable an elderly person to live independently as long as possible, only activating their caregiving team when necessary. One of the greatest fears of an elderly person is that something happens (a fall, a stroke) when they are alone. The solution, 24-hour care, is expensive and intrusive.
The Singapore Management University has been piloting sensor-enabled homes in Singapore through their SHINESeniors initiative. These sensors observe and analyze the elderly’s living patterns and immediately activate his care team when a change in pattern suggests a deterioration. Besides enabling independent living, this also allows companies and family members to allocate their time and resources efficiently.
Conclusion
Disrupting the flailing home care sector is essential to the quality of life of older folk, and the sustainability of healthcare systems when populations age. It’s a tough nut to crack, but I can’t think of a more important issue to work on right now, because our parents – and then us – are going to be the beneficiaries of positive disruption!
